Most clinicians who dream about opening their own practice think they need a massive war chest to make it happen. They picture inpatient facilities with round-the-clock nursing staff, medical equipment, fire safety inspections, and capital expenditures that would make a hospital CFO flinch.
Here's what they're missing: if you want to open an IOP/PHP program, you don't necessarily need beds, overnight staff, or hospital-style infrastructure—and the demand for structured outpatient care is being driven by big, measurable gaps in access and capacity (more on that below). The core appeal is simple: you're building a real clinical program, but with an operating model that looks a lot more like a normal business day than a 24/7 facility.
The Structural Advantage: What Makes IOP/PHP Different
The behavioral health treatment spectrum runs from weekly outpatient therapy on one end to inpatient psychiatric care on the other, and IOP/PHP sit in the middle of that continuum. In general, an IOP is commonly described as "more than 9 hours per week" for adults, while PHP is typically "20 or more hours per week," which is why PHP is considered the higher-intensity option. (ASAM Criteria overview)
That intensity matters operationally. Clients come in for structured group and individual services and then go home, which is the single biggest reason the cost structure is different from residential/inpatient. No beds means you typically avoid the operational realities that come with overnight care—continuous staffing, shift coverage, and the non-clinical services tied to housing.
IOP/PHP Startup Costs vs. Inpatient: The Numbers Tell the Story
Let's put some rough numbers on this so it's concrete.
Opening a residential or inpatient behavioral health facility often requires meaningfully more capital than an outpatient program because the facility must support 24-hour operations and life-safety needs tied to housing. Starting an intensive outpatient program, by contrast, can often be done with a smaller footprint and fewer "hard" build-out requirements, especially if you're leasing standard clinical office space rather than renovating bedrooms, kitchens, or residential common areas.
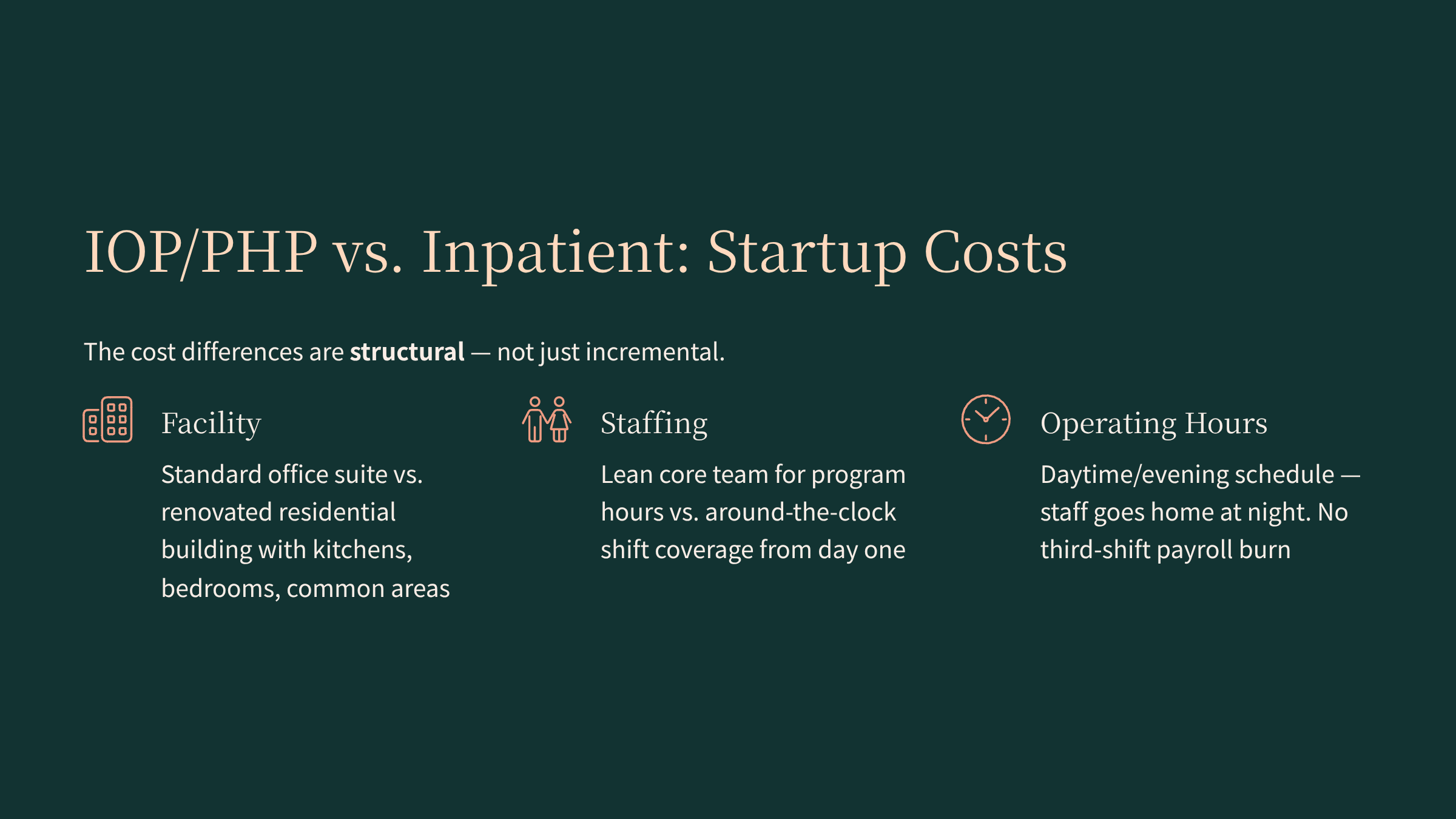
Here's where the cost differences stack up:
Facility Requirements
An IOP/PHP needs group therapy rooms, a few individual offices, a small reception area, and basic clinical admin space. In many markets, that can be done in a standard outpatient office suite—because you're not trying to operate a 24-hour living environment.
Staffing Model
Because IOP/PHP are scheduled, structured outpatient levels of care, you can typically launch with a leaner core team than a residential program requires. You're staffing program hours—not an around-the-clock milieu—so the baseline labor model is fundamentally different.
Operating Hours
Your program runs during the day (and/or evenings). Staff goes home at night. You're not building third-shift coverage into your payroll model from day one, which keeps early complexity and burn rate under control.
The Revenue Side Is Just as Compelling
Lower costs only matter if the revenue makes sense.
One useful anchor is Medicare's hospital outpatient prospective payment system (OPPS), where CMS sets per-diem payment methodologies for hospital outpatient PHP/IOP. For CY 2026, CMS finalized hospital-based per diem payments for IOP of $321.83 for days with three services and $421.67 for days with four or more services. (CMS CY 2026 OPPS/ASC final rule fact sheet; summary reported with figures in an OPPS analysis piece: HK Law OPPS update)
Commercial reimbursement varies widely by payer, state, and contracting structure, so any "typical rate" you hear should be treated as a market-dependent range rather than a guarantee. But the general business principle holds: when you combine structured attendance, higher weekly service intensity than standard outpatient, and a leaner operating model than inpatient, you can build a program where the unit economics work—especially once census stabilizes.
Why the Demand Is Exploding Right Now
The business case has gotten stronger because access gaps are real.
Federal workforce data shows the behavioral health system is dealing with substantial shortages across multiple roles and geographies, which directly constrains capacity. HRSA's State of the Behavioral Health Workforce, 2025 describes ongoing workforce challenges and highlights projected shortages across several behavioral health occupations. (HRSA workforce brief (2025))
In practical terms, when supply is tight, structured outpatient programs that can expand capacity without building a residential facility are often easier to stand up and scale.
Regulatory and Licensing: Simpler Than You Think
One of the biggest reasons clinicians hesitate to open an IOP/PHP program is the assumption that licensing and regulatory compliance will be impossibly complex.
It's not simple, but it's usually more manageable than residential/inpatient because you're not operating a 24/7 facility. That said, requirements vary significantly by state, and you should treat licensing timelines as variable rather than fixed—some states move quickly, others don't, and changes in staffing (especially medical director requirements) can affect readiness.
Insurance credentialing timelines also vary, and Medicare/Medicaid enrollment and commercial payer credentialing are not the same thing. If you're planning a launch, it's safest to assume credentialing and contracting can take months, and to structure your working capital accordingly.
What Clinicians Get Wrong About Starting an IOP
The biggest misconception isn't about money. It's about identity.
Many licensed clinicians assume running a business means abandoning clinical work. But an IOP/PHP is often small enough at launch that the founding clinician can stay clinically involved while the operation gets built—especially if you keep the model focused and avoid trying to do every level of care at once.
The operational complexity scales gradually. Billing, credentialing, compliance, and HR get heavier as you grow, but at the beginning, these are manageable if you approach them with a real plan and realistic timelines.
The IOP/PHP Playbook: What a Realistic Launch Looks Like
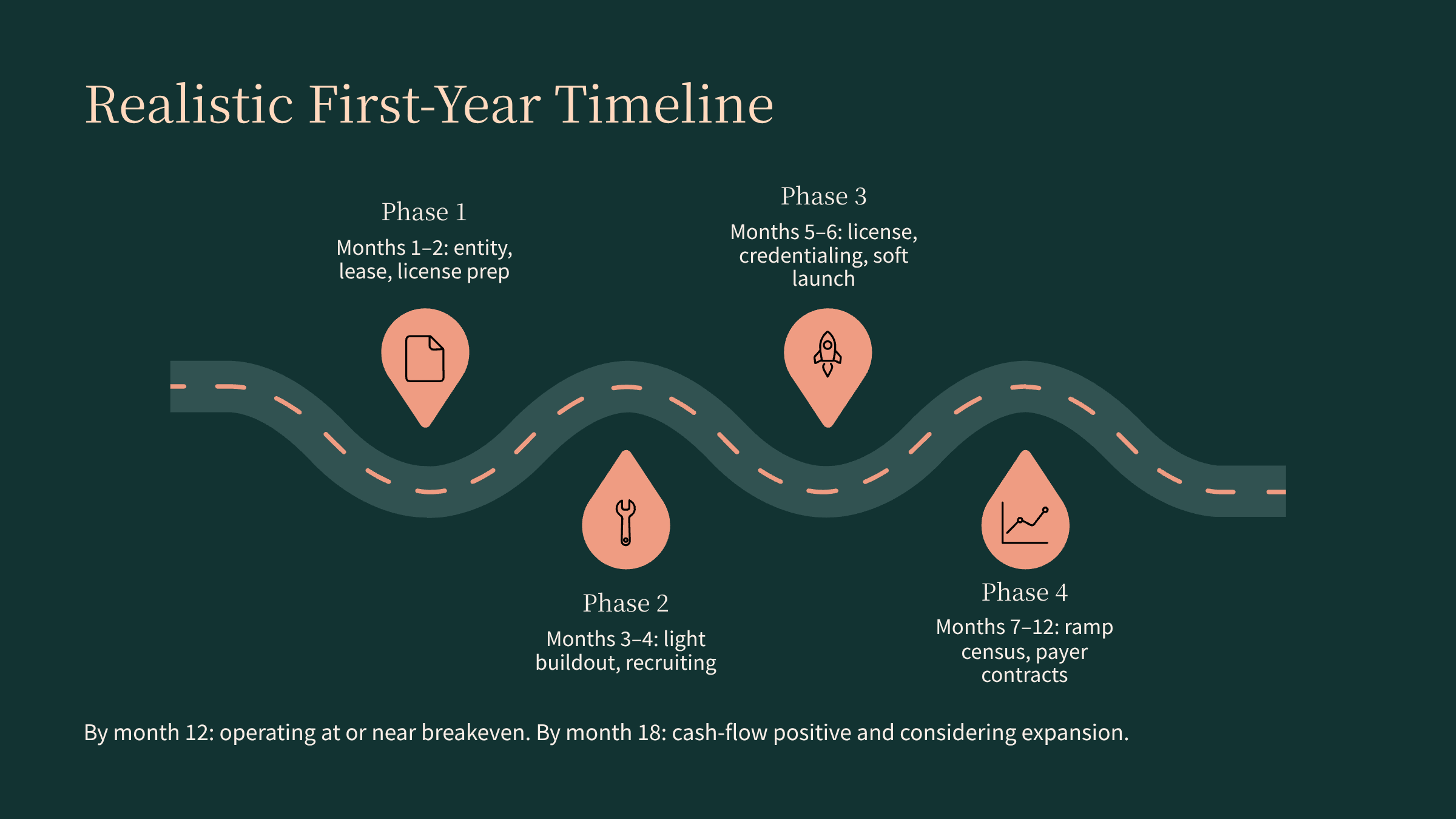
For clinicians and entrepreneurs who want to start an intensive outpatient program, here's what a realistic first-year timeline looks like:
Months 1–2: Entity formation, lease negotiation, license application submitted, clinical policies drafted.
Months 3–4: Facility buildout (light — mostly furniture and technology), credentialing applications submitted to target payers, staff recruiting begins.
Months 5–6: License obtained (in faster-moving states), first credentialing approvals start coming in, soft launch with private-pay or single-case agreements.
Months 7–12: Ramp to target census as additional payer contracts activate, referral relationships solidify, and the program builds a clinical reputation.
By month 12, a well-executed IOP launch should be operating at or near breakeven with a clear trajectory toward profitability. By month 18, strong programs are cash-flow positive and considering expansion—whether that's adding a PHP track, opening evening programming, or launching a second location.
FAQ
How much does it cost to open an IOP program?
Startup costs vary widely based on state licensing requirements, local rent, and how much staffing you hire before payer contracts go live. In general, IOPs tend to require less upfront capital than residential/inpatient because they don't involve 24/7 housing operations.
Do I need to be a doctor to open an IOP/PHP?
Not necessarily. Many states allow outpatient programs to be owned/operated by non-physician entities, but clinical governance, scope-of-practice rules, and medical oversight requirements (especially for PHP) can still apply—so you'll want to confirm requirements with your state licensing authority.
What is the difference between IOP and PHP?
IOP is commonly defined as more than 9 hours per week for adults, while PHP is typically 20 or more hours per week—so PHP is the higher-intensity level of care. (ASAM Criteria overview)
How long does it take to get licensed to run an IOP?
It depends on your state and the type of license you need, and timelines can change based on inspection schedules and application completeness. A safer planning assumption is that licensing and payer credentialing can take months, not weeks.
Is IOP/PHP profitable?
It can be. Medicare's OPPS provides one reference point for per-diem payment methodologies in hospital outpatient settings—for example, CMS finalized CY 2026 hospital-based IOP per diem payments of $321.83 (three services) and $421.67 (four or more services), which helps illustrate why structured outpatient care can support real revenue when attendance and documentation are strong. (CMS CY 2026 OPPS/ASC final rule fact sheet; figures also summarized here: HK Law OPPS update)
What states are best for opening an IOP/PHP?
There's no universal "best" state—what matters is licensing clarity, payer dynamics, and unmet need in your target community. Workforce constraints are widespread nationally, and federal data suggests shortages across many behavioral health occupations, which can create both demand pressure and hiring challenges depending on your market. (HRSA workforce brief (2025))
ForwardCare is a behavioral health MSO (Management Services Organization) that partners with clinicians to launch and scale IOP/PHP programs. They handle the business side — licensing support, insurance credentialing, billing, compliance, and operational infrastructure — so clinicians can focus on clinical care. If you're serious about opening an IOP/PHP program but don't want to figure out the business side alone, ForwardCare might be worth a conversation.

